The Saline Post - Saline Michigan Local News, Events, Classifieds and Alerts
Saline
Thu. Apr 25 2024
Marvin Fogle: 1944-2024
Saline Weather: Thursday April 25

High: 53°
Low: 29°
Wind: 4 MPH N
Chance of rain: 0%
Sunny, with a high of 53 and low of 29 degrees. Partly Cloudy in the morning, sunny for the afternoon, clear overnight.
Saline
Wed. Apr 24 2024
Mary Ploughman Remembered for Unwavering Spirit and Boundless Curiosity
Robison Bahnmiller Funeral Home
Contributor
Robison Bahnmiller Funeral Home
Contributor
Saline
Tue. Apr 23 2024
County Announces 4 Clean-up Days, All Require Registration
Tran Longmoore
Editor
Saline
Tue. Apr 23 2024
SOFTBALL: Cherry Homers, Triples as Saline Beats Pioneer
Tran Longmoore
Editor
Tran Longmoore
Editor
Tran Longmoore
Editor
Tran Longmoore
Editor
Tran Longmoore
Editor
Tran Longmoore
Editor
Saline
Thu. Apr 18 2024
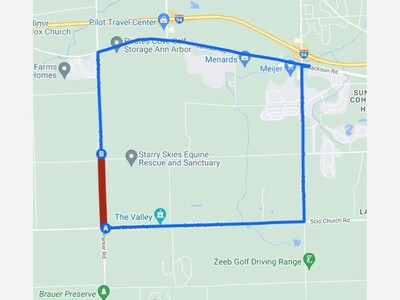
Resurfacing Work to Close Part of Parker Road Starting April 23
Tran Longmoore
Editor
Tran Longmoore
Editor
Saline
Wed. Apr 17 2024
Councillor Dillon Questions Messaging, Daytime Hydrant Flushing
Tran Longmoore
Editor
Tran Longmoore
Editor
Tran Longmoore
Editor
Brian Puffer
Contributor